What is acromegaly?
For most people, the body regulates hormones just like it’s supposed to. Nature expertly executes a careful balance, producing growth hormone (GH) in just the right amount at just the right time. But, for any number of reasons, things don’t always go as intended.
Acromegaly develops when a benign tumor grows on the pituitary gland and secretes increased levels of growth hormone (GH) during adulthood. As you might imagine, it’s a very rare disorder with an incidence of 3,000 new cases per year. There are about 25,000 acromegaly patients in the United States, and while it can develop at any age it usually affects middle-aged adults.
I really wish the awareness was more... unfortunately a lot of patients don't get the support they need or deserve.
— Jill
Clinical manifestations of acromegaly can vary, but in general the disease is characterized by somatic overgrowth (often bones in the hands, feet, and face), physical changes, multiple comorbidities (two or more medical conditions in a patient), and even premature mortality. These may be due to the direct effect of GH and/or IGF-1 (Insulin-like Growth Factor-1) on various organs and systems. Local effect of the tumor itself usually causes hypopituitarism (when a normal pituitary gland does not secrete the proper amount of hormones), or can cause visual problems.
Acromegaly treatment • 24 hours • 1 dose
The PATHFNDR studies are randomized, placebo-controlled, multi-center studies to evaluate the safety and efficacy of ONCE-DAILY, ORAL paltusotine in subjects with acromegaly. If you’d like to know more about these studies of this investigational drug, click here for more information and eligibility requirements.
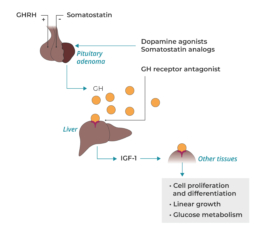
Pathophysiology
In normal pituitary function, Growth Hormone-Releasing Hormone (GHRH) stimulates the pituitary gland to secrete GH while the somatostatin hormone inhibits GH production. But in acromegaly, the micro- or macroadenoma is impervious to these regulatory instructions and secretes an increased level of GH. When the GH reaches the liver, it stimulates the liver to secrete increased levels of IGF-1. It is these increased IGF-1 levels that cause most of the metabolic dysfunction and somatic growth that present in acromegaly.
In a few people, acromegaly is caused by tumors in other parts of the body, such as the lungs or pancreas. Sometimes, these tumors secrete GH; in other cases they produce GHRH, which stimulates the pituitary to make more GH.2
Epidemiology
Prevalence
About 27,000 patients in the U.S.
Incidence rate
2,300 new cases per year
Median age at diagnosis
40.5 – 47 years
Acromegaly
The tumor that causes acromegaly is not only rare, but also very slow-growing, so physical changes occur over a period of several months, or even years. As a result, it can take a good while before patients notice anything is amiss, if they do at all. A common sign of acromegaly is enlarged hands and feet. Shoes that don’t fit anymore, tightening rings, or even more general symptoms like frequent headaches are chalked up to overwork, stress, or simply getting older. This puts the average time between the appearance of symptoms and diagnosis at 4.5 to 5 years. Other factors affecting proper, timely diagnosis include the patient’s geographical location and what type of healthcare practitioner he or she is seeing at the time.
A PATIENT’S VOICE
Before I was diagnosed, I saw probably ten doctors. I saw specialists and none of them caught it.
— Michelle
A variety of symptoms can occur
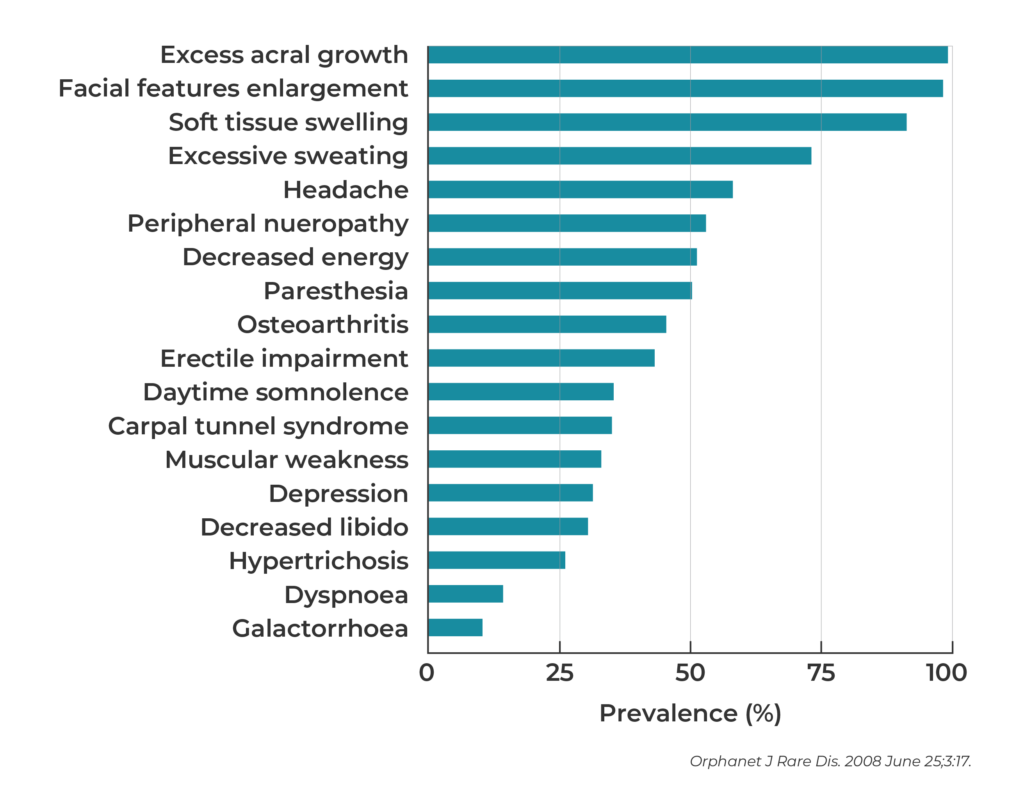
Because of the somatic growth caused by excessive amounts of IGF-1, some patients can appear considerably older than their chronological age. Common changes in facial appearance can include a larger nose, fuller lips, a protruding lower jaw and brow, more numerous skin folds, and a general appearance of being unwell.
Loss of peripheral vision is also possible as the patient’s macroadenoma compresses the optic chiasm. He or she may report newly developed difficulty parallel parking, though patients who don’t drive may not even notice this unless the performance of other everyday activities is adversely affected. Another presenting complaint is a sort of general fogginess. Patients have reported being forgetful – chronically misplacing car keys or losing debit cards. This chart4 shows the highly diverse range of acromegaly symptoms that patients can exhibit, another contributing factor in the longer-than-average time it takes to diagnose the condition.
Other possible symptoms
In addition to the above signs and symptoms, which vary from one patient to another, acromegaly may also cause:
-
- Coarse, oily, thickened skin
- Small outgrowths of skin tissue (skin tags)
- Severe snoring due to obstruction of the upper airway
- Enlarged tongue
- Pain and limited joint mobility
- Enlarged organs, such as the heart
| Presence of comorbidities at diagnosis5 | % of cases |
|---|---|
| Hypertension | 48 |
| Diabetes mellitus | 13 |
| Impaired glucose tolerance | 19 |
| Heart failure | 10 |
| Coronary artery disease | 8 |
Additional health problems are possible
Progression of acromegaly can result in other major health problems, which may include:6
More reasons why acromegaly can be difficult to diagnose
Contributing to the difficulty in diagnosis is the fact that patients themselves often go to different specialists in an attempt to figure out what’s wrong. If they’re suffering from tooth separation as a result of facial bone growth, they’ll consult a dentist. For joint pain they, naturally, go to an orthopedist. Vision problems will send them to an ophthalmologist and headaches will prompt a visit to a neurologist. Female patients may experience menstrual cycle irregularities, so they make an appointment with their gynecologist. Many of these specialists will not catch the root problem, so the patient’s acromegaly goes undiagnosed.
Often, the patient is alerted to the fact that something is off by someone who hasn’t seen them in a while. After all, a spouse who they live with every day is not likely to notice a change either. By contrast, a relative who comes for an infrequent visit may tell the patient, “You look different.” But an in-person visit isn’t even always necessary because the patient’s voice might sound different over the phone, since acromegaly affects cartilage as well. They’re told “I don’t even recognize your voice anymore.” Sometimes a patient will be alerted to a difference while looking through old pictures of themselves and noticing a change compared to more recent photos.
Recognize the signs and symptoms
The key is to familiarize yourself with the many different manifestations of acromegaly, as seen in the Signs and Symptoms section. Not all patients exhibit recognizable somatic growth, and successful early detection hinges on not relying on this as an exclusive criterion.
Check GH and IGF-1 levels
Endocrine Society clinical practice guidelines suggest screening for acromegaly by measurement of IGF-I in patients with typical clinical manifestations, but also in those who lack the typical clinical picture and have several associated conditions: sleep apnea syndrome, type 2 diabetes mellitus, debilitating arthritis, carpal tunnel syndrome, hyperhidrosis, and hypertension.7
Order an imaging study
Pituitary MRI studies reveal that only 25% of acromegaly patients are found to have a microadenoma (tumor diameter ≤10 mm). The rest have a macroadenoma (tumor diameter > 10 mm).
A PATIENT’S VOICE
I lived with acromegaly for 21 years before I was diagnosed.
— Rick
Anyone with this disease knows how debilitating it can be. The effects on patients’ lives are myriad:
Pain: The monthly injections hurt.
Disruption: Taking time off work, getting to the hospital/clinic and back, sitting in the waiting room, etc. It’s a chunk of nonproductive time that must be endured every single month. The stress and inconvenience get very old, very quickly.
Isolation: Physical symptoms such as somatic changes, fatigue, and depression cause patients to shrink their lives to fit their disease. The emotional components of isolation also play a debilitating role in their lives.
Frustration: The rarity of their disease, the time spent barking up the wrong trees with the wrong specialists, the lack of feasible treatments that fit their desired lifestyle, feeling like they’re not being heard, and the fact it took so long to get diagnosed can cause patients to become frustrated, angry, and depressed. This affects their entire families and loved ones, their friendships, and their careers.
A PATIENT’S VOICE
For a lot of patients, the changes in their body…facial changes especially… create a sense of wanting to hide themselves or not be as social.
— John
Treatment goals begin with reducing mortality and increasing quality of life by:8
- Reversing or reducing the severity/number of signs and symptoms
- Managing other diseases or conditions the patient may also have
- Restoring hormone levels to normal ranges with medical therapies
- Controlling tumor mass
- Maintaining optimum function of the pituitary gland
First and foremost, disease education is key. Because it is so rare, acromegaly is unfortunately often not detected or even suspected. Keeping it in mind as an option when patients present with symptoms will go a long way to getting them the treatment they need, sooner. Access to therapy is also critical, and there are different treatment options available, each with its own pros and cons.
A PATIENT’S VOICE
I went from a type A personality to a type Z, and honestly I lost some friends who just didn’t know how to deal with me anymore. I wasn’t always returning phone calls. I didn’t want to do a lot of the social things I did before the diagnosis.
— Traci
Surgery
At the time of detection, two-thirds of cases are macroadenomas. This may relate to diagnostic delays and poses challenges in the surgical management of these tumors.9 An endoscopic transsphenoidal resection of the tumor often reverses vision problems and restores normal hormone balance.9 In some cases, the surgeon is unable to remove the entire tumor, which could require further medical or radiation treatments. The remission rate of these macroadenomas is 48.6%.10
Medical therapy
Currently available pharmacological interventions11, 12 for the treatment of acromegaly can reduce a patient’s risk of complications and significantly improve characteristics of the condition. These include:
Dopamine agonists
- bromocriptine
- cabergoline
These oral drugs lower levels of GH and IGF-1 in some people. The tumor may decrease in size in some patients taking a dopamine agonist. Some people may develop nausea, vomiting and dizziness.
Somatostatin analogues
- octreotide-LAR
- lanreotide-ATG
- pasireotide-LAR
- oral octreotide
These drugs are synthetic versions of somatostatin and are usually administered by monthly injection. They act by suppressing the excessive secretion of GH by the pituitary tumor, reducing GH and IGF-1 levels.
GH receptor antagonist
- pegvisomant
This drug blocks the GH receptor in the liver, decreasing the secretion of IGF-1. According to treatment guidelines, it may be particularly helpful for patients who haven’t had good success with other treatments. Given as a daily injection, it can normalize IGF-1 levels and relieve symptoms in most acromegaly patients, but it doesn’t lower GH levels or reduce the tumor size.
The most common medical treatments are those administered by monthly injection. Delivered either intramuscularly or subcutaneously, these injections are quite painful and can be disruptive to a patient’s life. In addition to time-consuming travel to the clinic or hospital, some patients experience bruising, pain, and local site inflammation. Injections can also have imperfect efficacy because they are classically delivered via a depot preparation, so towards the end of the month some patients report returning symptoms as drug levels wane in their systems.
Oral octreotide eliminates some of the obstacles associated with injections. But it is short-acting and must be taken twice a day. It also requires patients to fast twice a day, making it both challenging and disruptive to adhere to a strict meal regimen. It may also interact with common medications for the treatment of diabetes and hypertension. Women taking birth control pills may need an additional contraceptive method.
Depending on the patient’s response, a combination of therapies may be used. A number of different side effects are possible. Please refer to product labeling for a complete list of side effects associated with any of these therapies.
Radiation therapy
Radiation therapy is indicated if medical treatment is unsuccessful. Because of the delayed effect, it may take years for it to noticeably improve acromegaly symptoms.13 The efficacy rate of this option is around 60% over ten years. In addition, the treatment could also affect the entirety of the pituitary gland, thus affecting all the other hormones it produces. This condition is called hypopituitarism and it requires lifelong hormonal replacement therapy.
As the primary goal of reducing mortality is determined by achieving normal levels of GH and IGF-1, periodic monitoring is recommended independent of the treatment option.
Paltusotine is the first once-daily, oral, selectively-targeted somatostatin receptor type 2 agonist in development for the proposed treatment of people with acromegaly. Paltusotine is an investigational drug candidate currently in clinical studies. The safety and efficacy of paltusotine have not been established. In clinical studies, paltusotine was well-tolerated with no severe or serious adverse events or new safety signals.
A PATIENT’S VOICE
My teeth were separating and it looked like I had a tooth missing. For years when I talked to anybody my mouth was closed; I didn’t smile. I wear a hat every time I go out because it did so much damage to my forehead and skull and I’m still self-conscious.
— Rick
The paltusotine timeline
March 2018
Initial results reported from a Phase 1, double-blind, randomized, placebo-controlled, single- and multiple-ascending dose trial to evaluate the safety, pharmacokinetics, and pharmacodynamics of paltusotine in 99 healthy volunteers.
Paltusotine demonstrated proof-of-concept (POC) by potently suppressing stimulated GH and baseline IGF-1 in these subjects. Plasma exposure of paltusotine indicated the drug was well-absorbed with a half-life of 42 to 50 hours, supporting once-daily administration in patients. The safety and tolerability of paltusotine observed in this trial was generally consistent with that of approved peptide somatostatin analogs.
August 2018
Submitted an Investigational New Drug (IND) application to the U.S. Food and Drug Administration (FDA).
Late 2018
Initiated two global Phase 2 clinical trials of paltusotine in acromegaly patients: ACROBAT EVOLVE and ACROBAT EDGE. Both completed their recruitment phase and were conducted at the same centers in the U.S. and globally. Patients who completed either study were eligible to participate in an open-label extension study (ACROBAT ADVANCE).
EVOLVE: Double-blind, placebo-controlled, randomized withdrawal study to evaluate the safety, efficacy, and pharmacokinetics of paltusotine compared to placebo in subjects with acromegaly who respond to octreotide LAR or lanreotide depot monotherapy.
EDGE: Open-label exploratory study to evaluate the safety, efficacy, and pharmacokinetics of paltusotine in subjects with acromegaly treated with somatostatin analog-based treatment regimens but who do not respond completely to monotherapy.
October 2020
Phase 2 ACROBAT and EDGE studies with paltusotine in acromegaly met primary endpoint.
1H 2021
We will begin a Phase 3 program in acromegaly.
2H 2021
We will begin a Phase 2 trial for the treatment of carcinoid syndrome associated with NETs.
Stay in the loop
Crinetics is committed to redefining what’s possible in the field of endocrinology. Patients are critical to our continued research in developing effective treatments for acromegaly and other rare endocrine diseases. If you or any of your patients are interested in our work and would like to stay informed by subscribing to our newsletter, The Better Bulletin, click here to subscribe.
Crinetics is intently focused on empowering acromegaly patients who are eager to be heard and who are seeking better treatment options, as well as all healthcare practitioners, to recognize the symptoms of acromegaly, diagnosis this rare disease, and implement the best course of treatment to control it.
We encourage you to establish connection with the following organizations to continue raising your awareness so that these vastly underserved patients can realize brighter futures. And, by all means, tell them Crinetics sent you.
The Final Word
Acromegaly is an insidious disease that urgently warrants greater awareness, and Crinetics is dedicated to making that happen. Your reading this web page is the first step in reaching our goal. If you’ve come this far, we appreciate you and we have a few final asks:
- Keep acromegaly in your mental Rolodex of possible diagnoses.
- Listen to patients who present with odd-sounding symptoms.
- Be the one who diagnoses it because you knew.
- Prescribe your patients the treatments that can help them feel better.
- Spread the word about this disease’s signs and symptoms.
- Connect with the pituitary/acromegaly community to keep on top of the latest treatments.
Let’s work together to bring these underserved patients Better therapies for Better lives.